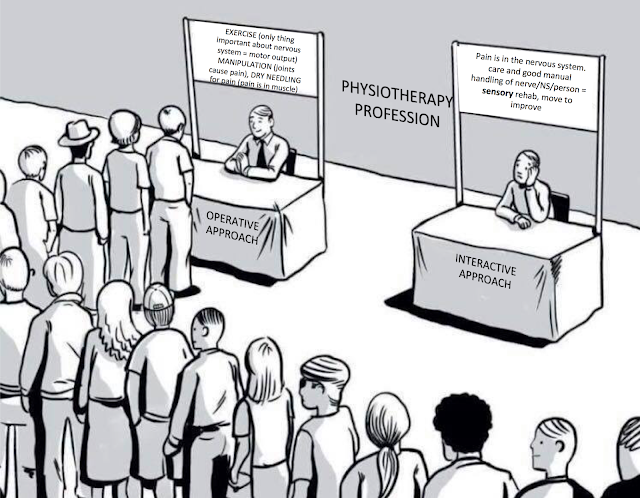
You know how all the literature on manual therapy says, when you read between the lines, is that it's "no better than placebo" ? Well, that's a good thing. It has taken away all the dreams from the dreamers, those who imagined their way of doing manual therapy was BETTER than any other way. Mostly this has deflated the orthopaedic manual therapy community, because of all the manual therapies out there, the practitioners (and studiers it must be emphasized) of OMPT were among the most strident about how much better their ways were than other kinds. Mostly though they were riding a wave of confirmation bias that sort of looked as follows:
1. People in pain often have impaired movement. Movement is important.
2. Movement is best measured at joints. Let's study the FX of our work by measuring ROM
3. Move the joints, bring back the movement. Pain should go away.
4. Voila, we have confirmed that pain comes from joints.
It became one of those closed loop ideas, self-referencing and self-confirming.
I never bought it, because in order to do OMPT properly you had to be able to feel joints and joint movement, so you could only do it on thin people, which a) left out all the fat people with pain and movement problems, and b) I knew I could help people of any size with their pain and movement problems without ever having to feel their joints, because I was working on their surfaces, not their depths, in the first place. In other words, I always found OMPT illogical.
In the end I feel vindicated because studies show there is no interrater reliability for palpation or diagnosis (too many type I errors). Good science shot down the myth that had grown that OMPT was superior.
We are straight back to non-specific FX again (of which placebo is just one kind, but not the entire story), which makes me glad. I embrace non-specific FX, because the hunt for specific FX from manual therapy has been futile.
Studies are starting to look like even orthopaedic surgery (for pain) is 'no better than placebo' for a lot of things.
If people are going to do things to other people that are 'no better than placebo', at least be kind! at least don't mess up their body even more!
On the other hand, there are all those studies that show major confirmation bias, like ones for needling and acupuncture showing good results. And just as many that say the results are NOT specific. Again, why be poking through skin with needles when toothpicks work just as well?
Taking the long view, that all manual therapy is non-specific, and that measuring an outcome does not prove an effect, I am more relaxed about doing this work than I ever was in the preceding 40 years, more willing to sit back and do non-specific things somewhat specifically, and let peoples' nervous systems do all their own heavy lifting to get themselves out of pain.
I'm totally willing to teach other people my set of tricks, that have sufficed for all these many years, plus new ones I have made up more recently, all the while telling students that they need to be adaptable and can make up their own new tricks, they have my blessing. Not that they need it. But they must FIRST sit through a very long lecture about the nervous system, its care and feeding, all the info I have about pain and brain mechanisms that pertain to manual therapy, with all the emphasis on the sensory portion, all the cutaneous nerves, so they will know what they are touching. And that they will be affecting the person, not the person's "body." And that they will accomplish more by doing less, and being kind while doing it, not hurting people more than they already hurt, unloading sore spots, not loading them more.
I'm totally willing to help people but I'm no longer willing to worry hard about trying to fix anybody. I do my best and that's all I need to do. I don't charge for results, I charge for my time. And inside the time people buy from me, I focus 100% on them, try to disconfirm all their noceboic beliefs, touch them very carefully and slowly and lightly where they hurt, load into them quite heavily where they don't hurt, and give their systems enough time to adapt until I can feel responsive changes in their physiology slow down and stop. Then I move on. Until the hour is up.
My results/outcomes have not been formally measured, but I would lay odds they are just as good as anyone else's.
.........
Old posts about non-specific FX:
Oct 20, 2012
May 15, 2014
May 20, 2014